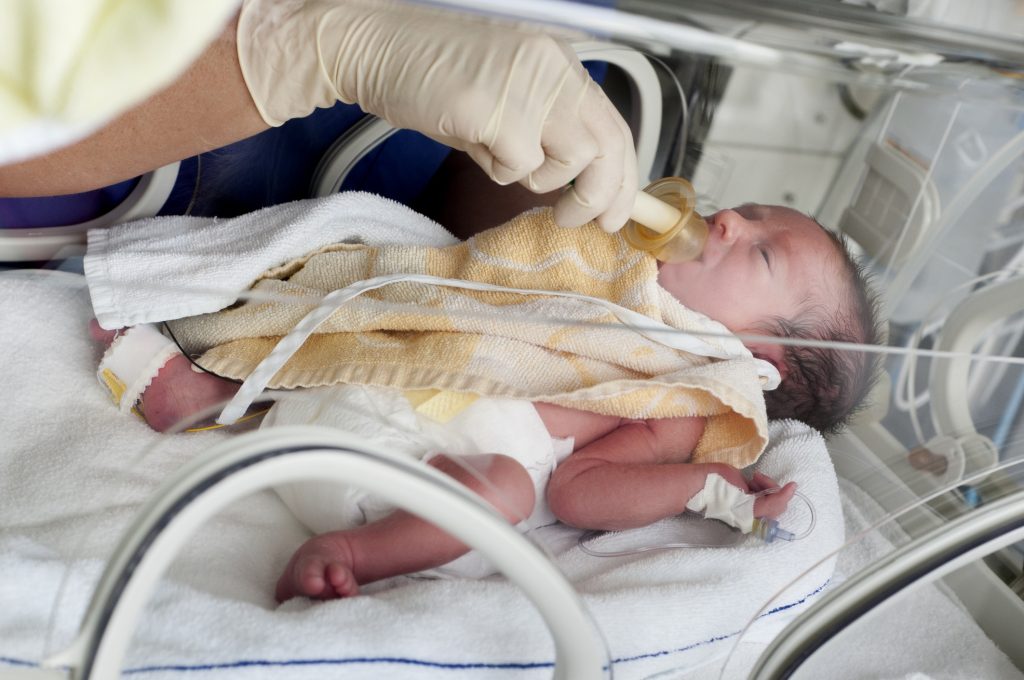
In the following interview, Michael Cabbad, MD, chair, Department of Obstetrics & Gynecology, and Director of Maternal Fetal Medicine at Richmond University Medical Center in Staten Island, discusses the medical complications pre-term babies can face, factors that can increase the risk of prematurity, and ways mothers can help prevent pre-term deliveries. Nearly 400,000 babies are born prematurely each year in the U.S.
How are pre-term deliveries defined and how prevalent are they?
Dr. Cabbad: With 39 weeks considered ‘full-term,’ ‘early term’ refers to delivery from 37 weeks to 38 weeks and six days, and anything prior to delivery before 37 weeks is considered ‘premature’ or ‘pre-term.’ According to the CDC, the rate of pre-term births in America was 10.5% in 2021, essentially meaning that a pre-term birth affected roughly one in every 10 U.S. infants born that year. The U.S. rate of pre-term birth mirrors that of the world rate, which currently stands at 10-11% according to the World Health Organization (WHO).
Michael Cabbad, MD, chair, Department of Obstetrics & Gynecology, and director of Maternal Fetal Medicine at Richmond University Medical Center in Staten Island
 What are some of the possible medical risks faced by babies born prematurely?
What are some of the possible medical risks faced by babies born prematurely?
Dr. Cabbad: Prematurity can potentially expose infants to many conditions – from respiratory distress syndrome, intraventricular hemorrhage, and bronchopulmonary dysplasia (BPD) to necrotizing colitis, retinopathy, apnea, cognitive delays, and motor performance difficulties. The degree to which these conditions can develop often correlates to how prematurely the baby delivers – e.g., the earlier the baby delivers, the greater the likelihood that any of these conditions may arise, with delivery prior to 32 weeks being the critical time frame when many of these things can occur.
When are pre-term deliveries medically appropriate or recommended?
Dr. Cabbad: There are many situations where pre-term delivery is medically indicated for the benefit of the mother and/or baby, such as if the mother has diabetes, hypertension, or has developed pre-eclampsia or a placental disorder, or if the baby is surrounded by excess amniotic fluid or develops any of a number of other fetal conditions.
What risk factors can predispose a woman to delivering prematurely?
Dr. Cabbad: Race is a factor; currently, the African American population has the highest risk of premature delivery, followed by Native Americans, Hispanics, those of Asian-Pacific descent, and Caucasians. Other risk factors include smoking, substance abuse, high levels of stress in the home and/or work environment, compromised social determinants of health (such as low economic status, limited education, poor eating habits, etc.), and the presence of periodontal disease. Being either overweight (with a body mass index, or BMI, over 30) or underweight (with a BMI less than 19.6) can also increase the risk of pre-term delivery, as can the presence of vaginal or sexually-transmitted infections, a history of spontaneous or induced abortion, use of fertilization technologies, cervical irregularities, and multiple gestation (twins, triplets, etc.). Finally, patients who begin prenatal care at a later point in their pregnancy are also at greater risk for pre-term delivery, making early prenatal care and intervention highly encouraged. Interestingly, while there are programs in place to help predict/identify those patients at risk for pre-term delivery, 50% of all patients who deliver pre-term have no predisposing factors.

How can women help reduce their risk of delivering prematurely?
Dr. Cabbad: Getting prenatal care early in the pregnancy and engaging in pregnancy planning with your doctor, especially if you have pre-disposing medical conditions, are strongly encouraged. Behaviors related to healthy living – such as eating well, getting adequate exercise, and reducing stress – are also highly recommended.
How are pre-term babies cared for at Richmond University Medical Center?
Dr. Cabbad: After identifying an individual at potential risk of pre-term delivery, collaborative efforts take place between our obstetricians, pediatricians, neonatologists, and nurses to monitor all of the physiological dynamics occurring within the child and provide the utmost respiratory, nutritional, and other support to the baby at a pace that supports its successful transition from the mother’s womb to the world. It’s a critical time that requires a whole team, including the parents, to be deeply involved and committed to the well-being of the child to help get them through that experience. Richmond University Medical Center has the specialists and support staff to expertly address these situations and the personalized, family-oriented care that they deliver to both mothers and babies is exceptional and truly helps so many premature babies turn out well. Thanks to the combined efforts of our team, technology, and the families involved, we’re able to help get babies through this critical and vulnerable time successfully.
Richmond University Medical Center’s Obstetrics and Gynecology Department can be reached at 718-818-3287 or by visiting www.rumcsi.org/obstetricsandgynecology. Richmond University Medical Center is located at 355 Bard Ave. and can be reached at 844- 934-CARE or by visiting www.rumcsi.org.
Susan Bloom